Quick Facts
More than 6 million Americans are living with Alzheimer's. By 2050, this number is projected to rise to nearly 13 million.

1 in 3 seniors dies with Alzheimer's or another dementia. It kills more than breast cancer and prostate cancer combined.

In 2023, Alzheimer’s and other dementias will cost the nation $345 billion. By 2050, these costs could rise to nearly $1 trillion.
Over 11 million Americans provide unpaid care for people with Alzheimer's or other dementias.

In 2022, unpaid caregivers provided an estimated 18 billion hours of care valued at $339.5 billion.
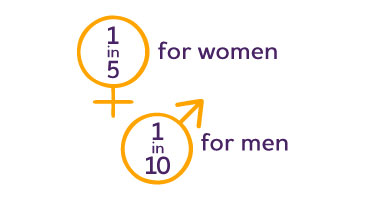
The lifetime risk for Alzheimer’s at age 45 is 1 in 5 for women and 1 in 10 for men.

Only 4 in 10 Americans would talk to their doctor right away when experiencing early memory or cognitive loss.

7 in 10 Americans would want to know early if they have Alzheimer's disease if it could allow for earlier treatment.

Between 2020 and 2030, 1.2 million additional direct care workers will be needed to care for the growing population of people living with dementia — the largest worker gap in the U.S.
Prevalence
 The number of Americans living with Alzheimer's is growing — and growing fast. More than 6 million Americans of all ages have Alzheimer's.
The number of Americans living with Alzheimer's is growing — and growing fast. More than 6 million Americans of all ages have Alzheimer's.
An estimated 6.7 million Americans age 65 and older are living with Alzheimer's in 2023. Seventy-three percent are age 75 or older.
- About 1 in 9 people age 65 and older (10.7%) has Alzheimer's.
- Almost two-thirds of Americans with Alzheimer's are women.
- Older Black Americans are about twice as likely to have Alzheimer's or other dementias as older Whites.
- Older Hispanics are about one and one-half times as likely to have Alzheimer's or other dementias as older Whites.
As the size of the U.S. population age 65 and older continues to grow, so too will the number and proportion of Americans with Alzheimer’s or other dementias. By 2050, the number of people age 65 and older with Alzheimer’s may grow to a projected 12.7 million, barring the development of medical breakthroughs to prevent or cure Alzheimer’s disease.
Get Involved
Volunteer, fundraise, advocate and more — you can make a difference in the lives of people affected by Alzheimer’s.
Mortality
 Alzheimer’s is not just memory loss. Alzheimer’s kills.
Alzheimer’s is not just memory loss. Alzheimer’s kills.
- 1 in 3 seniors dies with Alzheimer's or another dementia. It kills more than breast cancer and prostate cancer combined.
- Deaths from Alzheimer’s have more than doubled between 2000 and 2019, while those from heart disease — the leading cause of death — have decreased.
- At age 70, seniors living with Alzheimer's are twice as likely to die before age 80 than those who do not have the disease.
People age 65 and older survive an average of four to eight years after a diagnosis of Alzheimer’s, yet some live as long as 20 years with Alzheimer’s. This reflects the slow, uncertain progression of the disease.
Invest in the Fight to End Alzheimer’s
The first survivor of Alzheimer’s is out there, but we won’t get there without you.
Caregivers
 Eighty-three percent of the help provided to older adults in the U.S. comes from family members, friends or other unpaid caregivers. Nearly half of all caregivers who provide help to older adults do so for someone living with Alzheimer's or another dementia.
Eighty-three percent of the help provided to older adults in the U.S. comes from family members, friends or other unpaid caregivers. Nearly half of all caregivers who provide help to older adults do so for someone living with Alzheimer's or another dementia.
Who are the caregivers?
- About 30% of caregivers are age 65 or older.
- Nearly half of all caregivers (48%) who provide help to older adults do so for someone living with Alzheimer's or another dementia.
- Approximately two-thirds of caregivers are women. More specifically, over one-third of dementia caregivers are daughters.
- Approximately one-quarter of dementia caregivers are “sandwich generation” caregivers — meaning that they care not only for an aging parent but also for at least one child.
- Forty-one percent of caregivers have a household income of $50,000 or less.
Alzheimer's takes a devastating toll on caregivers. Compared with caregivers of people without dementia, twice as many caregivers of those with dementia indicate substantial emotional, financial and physical difficulties.
Of the total lifetime cost of caring for someone with dementia, 70% is borne by families — either through out-of-pocket health and long-term care expenses or from the value of unpaid care.
Caring for Someone with Alzheimer’s?
Get the support you need to handle the day-to-day, plan for the future and help you live well.
Workforce
 As the prevalence of Alzheimer’s disease increases, so does the need for additional members of the paid workforce who are involved in diagnosing, treating and caring for those living with the disease.
As the prevalence of Alzheimer’s disease increases, so does the need for additional members of the paid workforce who are involved in diagnosing, treating and caring for those living with the disease.
- Even though the vast majority of initial diagnoses are made by primary care physicians (PCPs), nearly 40% reported that they were "never" or "only sometimes" comfortable making a diagnosis of Alzheimer's or another dementia.
- Half of PCPs reported that they do not feel adequately prepared to care for individuals with Alzheimer’s and other dementias, and more than 25% reported being “only sometimes” or “never” comfortable answering patient questions about dementia.
- The U.S. will have to nearly triple the number of geriatricians to effectively care for the number of people projected to have Alzheimer's in 2050.
- Few care professionals specialize in geriatrics:
- Only 12% of nurse practitioners have special expertise in gerontological care.
- Less than 1% of registered nurses, physician assistants and pharmacists identify themselves as specializing in geriatrics.
- Only 4% of social workers have formal certification in geriatric social work.
- The demand for direct care workers (roles such as nurses aides and home health aides) is projected to grow by more than 40% between 2016 and 2026, while their availability is expected to decline.
- Turnover rates for direct care workers are high — estimated at 64% annually for those providing home care and 99% for nursing assistants in nursing homes.
Be Prepared and Talk to Your Doctor
Effective communication with your doctor is important when you are seeking a diagnosis for memory loss. Be prepared to ask questions and be as honest as possible.
Cost to the Nation
 The costs of health care and long-term care for individuals living with Alzheimer’s or other dementias are substantial, and dementia is one of the costliest conditions to society.
The costs of health care and long-term care for individuals living with Alzheimer’s or other dementias are substantial, and dementia is one of the costliest conditions to society.
In 2023, Alzheimer's and other dementias will cost the nation $345 billion — not including the value of unpaid caregiving. Medicare and Medicaid are expected to cover $222 billion (64%), while out-of-pocket spending is expected to be $87 billion. Total payments for health care, long-term care and hospice care for people living with dementia are projected to increase to nearly $1 trillion in 2050.
- The total lifetime cost of care for a person living with dementia is estimated at $392,874.
- People living with Alzheimer's or other dementias have twice as many hospital stays per year as other older people.
- Medicare beneficiaries with Alzheimer's or other dementias are more likely than those without dementia to have other chronic conditions, such as heart disease, diabetes and kidney disease.
- Older people living with Alzheimer’s or other dementias have more skilled nursing facility stays and home health care visits per year than other older people.
- People living with Alzheimer's or other dementias make up a large proportion of all elderly people who receive adult day services and nursing home care.
Take Action
Ending Alzheimer's is possible — Congress can make it happen. Join us and help make Alzheimer’s a national priority.
Special Report — The Patient Journey in an Era of New Treatments
 The Food and Drug Administration (FDA) approval of two new treatment options has generated excitement and hope for individuals with mild cognitive impairment (MCI) or mild dementia due to Alzheimer’s disease, and their families. In order to receive better care, it is essential for patients to have conversations about memory concerns with their health care providers as early as possible, and for the physician workforce to be adequately prepared to handle diagnosis, care and eventual treatment of Alzheimer's and other dementias.
The Food and Drug Administration (FDA) approval of two new treatment options has generated excitement and hope for individuals with mild cognitive impairment (MCI) or mild dementia due to Alzheimer’s disease, and their families. In order to receive better care, it is essential for patients to have conversations about memory concerns with their health care providers as early as possible, and for the physician workforce to be adequately prepared to handle diagnosis, care and eventual treatment of Alzheimer's and other dementias.
The unfortunate reality, as reported by The Patient Journey in an Era of New Treatments, is that most Americans are reluctant to see a doctor early and tend to wait until the symptoms have a noticeable impact on their lives.
- Only 40% of Americans say they would talk to their doctor right away when experiencing symptoms of MCI. Many dismiss changes in memory as "normal aging."
- At the same time, 70% of Americans said they would want to know early if they have Alzheimer's disease if it could allow for earlier treatment.
- Participants listed persistent challenges with communicating effectively with their PCP, including:
- Emotional reactions and limited vocabulary to express cognitive issues.
- Perceived risks — like receiving an incorrect diagnosis, learning of a serious health problem and receiving unnecessary treatment — outweighing the benefits.
- Assumptions about what doctors will say and do.
- A desire for inclusive, culturally appropriate conversations and shared decision-making.
- A preference to discuss cognitive issues with friends instead of medical professionals or family.
- Physicians are not taking the initiative to talk with patients either. Nearly all PCPs report waiting for patients (97%) or family members (98%) to make them aware of symptoms or request an assessment.
If those with cognitive concerns overcome their hesitations, the first medical professional many people approach is their primary care provider. But PCPs report lack of time and confidence in diagnosing and caring for people with Alzheimer's or another dementia. Instead, they refer patients to specialists, who may or may not be accessible. The shortage of specialists or specialists who are at capacity and no longer accepting new patients is likely to have the most immediate and obvious impact on people at the MCI phase of Alzheimer's disease who may be eligible for newly-approved treatments.
- Twenty U.S. states have been termed "dementia neurology deserts," which means that they are projected to have fewer than 10 neurologists per 10,000 people with dementia in 2025.
- The U.S. will have to nearly triple the number of geriatricians who were practicing in 2021 to effectively care for the approximately 10% of those 65 and older who are projected to have Alzheimer’s dementia in 2050.
- 44% of PCPs in large cities, 54% in suburban areas near large cities, 63% in small cities or towns, and 71% of PCPs in rural areas reported that there were not enough specialists in their area.
Beyond the need for more specialists in the field of dementia care, continuing to educate communities about memory, thinking problems and health care in this era of new and emerging treatments is key.
Read The Patient Journey in an Era of New Treatments and view the special report infographic.
Learn How to Navigate Your Treatment Options
Progress in Alzheimer's research has created promising new treatments. Learn about the different drugs so you can discuss the options with a doctor.