Appropriateness of Percutaneous Coronary Interventions in Patients With Stable Coronary Artery Disease in US Department of Veterans Affairs Hospitals From 2013 to 2015
- PMID: 32315067
- PMCID: PMC7175080
- DOI: 10.1001/jamanetworkopen.2020.3144
Appropriateness of Percutaneous Coronary Interventions in Patients With Stable Coronary Artery Disease in US Department of Veterans Affairs Hospitals From 2013 to 2015
Abstract
Importance: In hospitals outside of the US Department of Veterans Affairs (VA) system, 1 in 10 percutaneous coronary interventions (PCIs) for stable coronary artery disease is considered rarely appropriate by the appropriate use criteria, with variation across hospitals. The appropriateness of PCIs in VA hospitals has not been documented.
Objective: To characterize the appropriateness of PCIs in VA hospitals.
Design, setting, and participants: This retrospective cohort study included patients with stable coronary artery disease undergoing elective PCI from November 1, 2013, to October 31, 2015, within the VA Clinical Assessment, Reporting, and Tracking Program, an operational program that includes 59 VA hospitals. Data were analyzed from March 1, 2019, to August 8, 2019.
Exposures: Elective PCI at a VA hospital.
Main outcomes and measures: Proportion of PCIs classified as appropriate, may be appropriate, or rarely appropriate; extent of hospital-level variation in rarely appropriate PCIs using criteria issued by cardiovascular professional societies in 2012. The extent of hospital-level variation in rates of rarely appropriate PCI was characterized using hospital proportions and random-effect logistic regression.
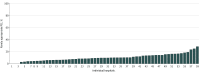
Results: Among 2611 patients undergoing elective PCI (mean [SD] age, 66.3 [7.6] years; 2577 [98.7%] men) at 59 hospitals, a total of 778 PCIs (29.8%) were classified as appropriate, 1561 PCIs (59.8%) were classified as may be appropriate, and 272 PCIs (10.4%) were classified as rarely appropriate. Rarely appropriate PCIs were more commonly performed in patients who had low-risk stress test findings (220 patients [89.1%]), who were taking no (100 patients [36.8%]) or 1 (167 patients [61.4%]) antianginal medication, or who had 1 coronary artery stenosis (185 patients [68.0%]). The unadjusted hospital-level rates of rarely appropriate PCIs ranged from 0% to 28.6%, with a median (interquartile range) of 9.7% (6.3%-13.9%). Random-effect models yielded an estimated median (interquartile range) rate of rarely appropriate PCI of 10.4% (8.7%-12.3%).
Conclusions and relevance: These findings suggest that in VA practice, most PCIs for stable coronary artery disease were classified as appropriate or may be appropriate. However, 1 in 10 PCIs was classified as rarely appropriate, with variation across VA hospitals. Efforts to improve patient selection are needed.
Conflict of interest statement
Figures
Similar articles
-
Comparison of Accessibility, Cost, and Quality of Elective Coronary Revascularization Between Veterans Affairs and Community Care Hospitals.JAMA Cardiol. 2018 Feb 1;3(2):133-141. doi: 10.1001/jamacardio.2017.4843. JAMA Cardiol. 2018. PMID: 29299607 Free PMC article.
-
Stress Testing After Percutaneous Coronary Intervention in the Veterans Affairs HealthCare System: Insights from the Veterans Affairs Clinical Assessment, Reporting, and Tracking Program.Circ Cardiovasc Qual Outcomes. 2015 Sep;8(5):486-92. doi: 10.1161/CIRCOUTCOMES.114.001561. Epub 2015 Jul 21. Circ Cardiovasc Qual Outcomes. 2015. PMID: 26198400
-
Comparative Outcomes After Percutaneous Coronary Intervention Among Black and White Patients Treated at US Veterans Affairs Hospitals.JAMA Cardiol. 2017 Sep 1;2(9):967-975. doi: 10.1001/jamacardio.2017.2180. JAMA Cardiol. 2017. PMID: 28724126 Free PMC article.
-
Trends in Coded Indications for Percutaneous Coronary Interventions in Medicare and the Veterans Affairs After Implementation of Hospital-Level Reporting of Appropriate Use Criteria.Circ Cardiovasc Qual Outcomes. 2021 Apr;14(4):e006887. doi: 10.1161/CIRCOUTCOMES.120.006887. Epub 2021 Mar 15. Circ Cardiovasc Qual Outcomes. 2021. PMID: 33719490
-
1-year risk-adjusted mortality and costs of percutaneous coronary intervention in the Veterans Health Administration: insights from the VA CART Program.J Am Coll Cardiol. 2015 Jan 27;65(3):236-42. doi: 10.1016/j.jacc.2014.10.048. J Am Coll Cardiol. 2015. PMID: 25614420
Cited by 4 articles
-
The reduction of race and gender bias in clinical treatment recommendations using clinician peer networks in an experimental setting.Nat Commun. 2021 Nov 15;12(1):6585. doi: 10.1038/s41467-021-26905-5. Nat Commun. 2021. PMID: 34782636 Free PMC article.
-
Appropriate use criteria for coronary angiography: a single centre experience.Int J Cardiol Heart Vasc. 2020 Nov 30;31:100677. doi: 10.1016/j.ijcha.2020.100677. eCollection 2020 Dec. Int J Cardiol Heart Vasc. 2020. PMID: 33304989 Free PMC article.
-
Outcomes in CME/CPD - Special Collection: How to make the "pyramid" a perpetuum mobile.J Eur CME. 2020 Oct 27;9(1):1832750. doi: 10.1080/21614083.2020.1832750. J Eur CME. 2020. PMID: 33194316 Free PMC article.
-
Association Between Elective Percutaneous Coronary Intervention Appropriateness and Publicly Reported Outcomes.Circ Cardiovasc Qual Outcomes. 2021 Jan;14(1):e007421. doi: 10.1161/CIRCOUTCOMES.120.007421. Epub 2020 Nov 9. Circ Cardiovasc Qual Outcomes. 2021. PMID: 33161758 Free PMC article. No abstract available.
References
-
- Dagenais GR, Lu J, Faxon DP, et al. ; Bypass Angioplasty Revascularization Investigation 2 Diabetes (BARI 2D) Study Group . Effects of optimal medical treatment with or without coronary revascularization on angina and subsequent revascularizations in patients with type 2 diabetes mellitus and stable ischemic heart disease. Circulation. 2011;123(14):1492-1500. doi:10.1161/CIRCULATIONAHA.110.978247 - DOI - PubMed
Publication types
MeSH terms
Grant support
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous