Comparison of Accessibility, Cost, and Quality of Elective Coronary Revascularization Between Veterans Affairs and Community Care Hospitals
- PMID: 29299607
- PMCID: PMC5838592
- DOI: 10.1001/jamacardio.2017.4843
Comparison of Accessibility, Cost, and Quality of Elective Coronary Revascularization Between Veterans Affairs and Community Care Hospitals
Abstract
Importance: The Veterans Affairs (VA) Community Care (CC) Program supplements VA care with community-based medical services. However, access gains and value provided by CC have not been well described.
Objectives: To compare the access, cost, and quality of elective coronary revascularization procedures between VA and CC hospitals and to evaluate if procedural volume or publicly reported quality data can be used to identify high-value care.
Design, setting, and participants: Observational cohort study of veterans younger than 65 years undergoing an elective coronary revascularization, controlling for differences in risk factors using propensity adjustment. The setting was VA and CC hospitals. Participants were veterans undergoing elective percutaneous coronary intervention (PCI) and veterans undergoing coronary artery bypass graft (CABG) procedures between October 1, 2008, and September 30, 2011. The analysis was conducted between July 2014 and July 2017.
Exposures: Receipt of an elective coronary revascularization at a VA vs CC facility.
Main outcomes and measures: Access to care as measured by travel distance, 30-day mortality, and costs.
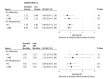
Results: In the 3 years ending on September 30, 2011, a total of 13 237 elective PCIs (79.1% at the VA) and 5818 elective CABG procedures (83.6% at the VA) were performed in VA or CC hospitals among veterans meeting study inclusion criteria. On average, use of CC was associated with reduced net travel by 53.6 miles for PCI and by 73.3 miles for CABG surgery compared with VA-only care. Adjusted 30-day mortality after PCI was higher in CC compared with VA (1.54% for CC vs 0.65% for VA, P < .001) but was similar after CABG surgery (1.33% for CC vs 1.51% for VA, P = .74). There were no differences in adjusted 30-day readmission rates for PCI (7.04% for CC vs 7.73% for VA, P = .66) or CABG surgery (8.13% for CC vs 7.00% for VA, P = .28). The mean adjusted PCI cost was higher in CC ($22 025 for CC vs $15 683 for VA, P < .001). The mean adjusted CABG cost was lower in CC ($55 526 for CC vs $63 144 for VA, P < .01). Neither procedural volume nor publicly reported mortality data identified hospitals that provided higher-value care with the exception that CABG mortality was lower in small-volume CC hospitals.
Conclusions and relevance: In this veteran cohort, PCIs performed in CC hospitals were associated with shorter travel distance but with higher mortality, higher costs, and minimal travel savings compared with VA hospitals. The CABG procedures performed in CC hospitals were associated with shorter travel distance, similar mortality, and lower costs. As the VA considers expansion of the CC program, ongoing assessments of value and access gains are essential to optimize veteran outcomes and VA spending.
Conflict of interest statement
Figures

Comment in
-
Coronary Revascularization for Veterans-There's No Place Like Home.JAMA Cardiol. 2018 Feb 1;3(2):142-143. doi: 10.1001/jamacardio.2017.4864. JAMA Cardiol. 2018. PMID: 29299608 No abstract available.
-
Importance of Objectively Comparing Local VA and Non-VA Care and Outcomes: Serving Veterans Well.JAMA Cardiol. 2018 May 1;3(5):443. doi: 10.1001/jamacardio.2018.0338. JAMA Cardiol. 2018. PMID: 29590336 No abstract available.
Similar articles
-
Federal Payments for Coronary Revascularization Procedures Among Dual Enrollees in Medicare Advantage and the Veterans Affairs Health Care System.JAMA Netw Open. 2020 Apr 1;3(4):e201451. doi: 10.1001/jamanetworkopen.2020.1451. JAMA Netw Open. 2020. PMID: 32250432 Free PMC article.
-
Same-day discharge among patients undergoing elective PCI: Insights from the VA CART Program.Am Heart J. 2019 Dec;218:75-83. doi: 10.1016/j.ahj.2019.09.003. Epub 2019 Sep 12. Am Heart J. 2019. PMID: 31707331
-
Patient access and 1-year outcomes of percutaneous coronary intervention facilities with and without on-site cardiothoracic surgery: insights from the Veterans Affairs (VA) Clinical Assessment, Reporting, and Tracking (CART) program.Circulation. 2014 Oct 14;130(16):1383-91. doi: 10.1161/CIRCULATIONAHA.114.009713. Epub 2014 Sep 4. Circulation. 2014. PMID: 25189215
-
Evidence Brief: Comparative Effectiveness of Appointment Recall Reminder Procedures for Follow-up Appointments.2015 Jul. In: VA Evidence Synthesis Program Evidence Briefs [Internet]. Washington (DC): Department of Veterans Affairs (US); 2011–. 2015 Jul. In: VA Evidence Synthesis Program Evidence Briefs [Internet]. Washington (DC): Department of Veterans Affairs (US); 2011–. PMID: 27606388 Free Books & Documents. Review.
-
Comparing cost aspects of coronary artery bypass graft surgery with coronary artery stenting.J Cardiovasc Surg (Torino). 2012 Oct;53(5):641-50. Epub 2012 Jan 17. J Cardiovasc Surg (Torino). 2012. PMID: 22252542 Review.
Cited by 8 articles
-
Patient and hospital factors associated with 30-day readmissions after coronary artery bypass graft (CABG) surgery: a systematic review and meta-analysis.J Cardiothorac Surg. 2021 Jun 10;16(1):172. doi: 10.1186/s13019-021-01556-1. J Cardiothorac Surg. 2021. PMID: 34112216 Free PMC article.
-
The relationship between procedural volume and patient outcomes for percutaneous coronary interventions: a systematic review and meta-analysis.HRB Open Res. 2021 Jan 28;4:10. doi: 10.12688/hrbopenres.13203.1. eCollection 2021. HRB Open Res. 2021. PMID: 33842830 Free PMC article.
-
Performance of the Veterans Choice Program for Improving Access to Colonoscopy at a Tertiary VA Facility.Fed Pract. 2020 May;37(5):224-228. Fed Pract. 2020. PMID: 32454576 Free PMC article.
-
Association of Cardiac Rehabilitation With Survival Among US Veterans.JAMA Netw Open. 2020 Mar 2;3(3):e201396. doi: 10.1001/jamanetworkopen.2020.1396. JAMA Netw Open. 2020. PMID: 32196104 Free PMC article.
-
Characteristics of the Quality Improvement Content of Cardiac Catheterization Peer Reviews in the Veterans Affairs Clinical Assessment, Reporting, and Tracking Program.JAMA Netw Open. 2019 Aug 2;2(8):e198393. doi: 10.1001/jamanetworkopen.2019.8393. JAMA Netw Open. 2019. PMID: 31373652 Free PMC article.
References
-
- Department of Veterans Affairs . Expanded access to non-VA care through the Veterans Choice Program: interim final rule. Fed Regist. 2015;80(230):74991-74996. - PubMed
-
- Giroir BP, Wilensky GR. Reforming the Veterans Health Administration: beyond palliation of symptoms. N Engl J Med. 2015;373(18):1693-1695. - PubMed
-
- Health Net Federal Services . About Veterans Choice Program. https://www.hnfs.com/content/hnfs/home/va/provider/veterans-choice-progr.... Accessed June 30, 2017.
Publication types
MeSH terms
Grant support
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

