Seizures are a druggable mechanistic link between TBI and subsequent tauopathy
- PMID: 33527898
- PMCID: PMC7853719
- DOI: 10.7554/eLife.58744
Seizures are a druggable mechanistic link between TBI and subsequent tauopathy
Abstract
Traumatic brain injury (TBI) is a prominent risk factor for dementias including tauopathies like chronic traumatic encephalopathy (CTE). The mechanisms that promote prion-like spreading of Tau aggregates after TBI are not fully understood, in part due to lack of tractable animal models. Here, we test the putative role of seizures in promoting the spread of tauopathy. We introduce 'tauopathy reporter' zebrafish expressing a genetically encoded fluorescent Tau biosensor that reliably reports accumulation of human Tau species when seeded via intraventricular brain injections. Subjecting zebrafish larvae to a novel TBI paradigm produced various TBI features including cell death, post-traumatic seizures, and Tau inclusions. Bath application of dynamin inhibitors or anticonvulsant drugs rescued TBI-induced tauopathy and cell death. These data suggest a role for seizure activity in the prion-like seeding and spreading of tauopathy following TBI. Further work is warranted regarding anti-convulsants that dampen post-traumatic seizures as a route to moderating subsequent tauopathy.
Keywords: anti-epileptics; epilepsy; neuroscience; neurotrauma; post-traumatic seizures; tauopathy; traumatic brain injury; zebrafish.
Plain language summary
Traumatic brain injury can result from direct head concussions, rapid head movements, or a blast wave generated by an explosion. Traumatic brain injury often causes seizures in the short term and is a risk factor for certain dementias, including Alzheimer’s disease and chronic traumatic encephalopathy in the long term. A protein called Tau undergoes a series of chemical changes in these dementias that makes it accumulate, form toxic filaments and kill neurons. The toxic abnormal Tau proteins are initially found only in certain regions of the brain, but they spread as the disease progresses. Previous studies in Alzheimer’s disease and other diseases where Tau proteins are abnormal suggest that Tau can spread between neighboring neurons and this can be promoted by neuron activity. However, scientists do not know whether similar mechanisms are at work following traumatic brain injury. Given that seizures are very common following traumatic brain injury, could they be partly responsible for promoting dementia? To investigate this, researchers need animal models in which they can measure neural activity associated with traumatic brain injury and observe the spread of abnormal Tau proteins. Alyenbaawi et al. engineered zebrafish so that their Tau proteins would be fluorescent, making it possible to track the accumulation of aggregated Tau protein in the brain. Next, they invented a simple way to perform traumatic brain injury on zebrafish larvae by using a syringe to produce a pressure wave. After this procedure, many of the fish exhibited features consistent with progression towards dementia, and seizure-like behaviors. The results showed that post-traumatic seizures are linked to the spread of aggregates of abnormal Tau following traumatic brain injury. Alyenbaawi et al. also found that anticonvulsant drugs can lower the levels of abnormal Tau proteins in neurons, preventing cell death, and could potentially ameliorate dementias associated with traumatic brain injury. These drugs are already being used to prevent post-traumatic epilepsy, but more research is needed to confirm whether they reduce the risk or severity of Tau-related neurodegeneration.
Conflict of interest statement
HA, RK, LL, RK, MD, QB, HW, EB, WA No competing interests declared
Figures








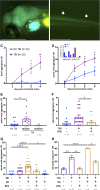
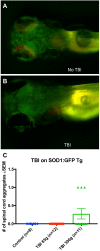







Comment in
-
Visualizing traumatic brain injuries.Elife. 2021 Feb 2;10:e65676. doi: 10.7554/eLife.65676. Elife. 2021. PMID: 33527900 Free PMC article.
-
Treating Post-Traumatic Seizures to Limit Tau Accumulation in Larval Zebrafish.Epilepsy Curr. 2021 Apr 29;21(4):285-286. doi: 10.1177/15357597211012961. eCollection 2021 Jul-Aug. Epilepsy Curr. 2021. PMID: 34690568 Free PMC article. No abstract available.
Similar articles
-
Prion-Like Propagation Mechanisms in Tauopathies and Traumatic Brain Injury: Challenges and Prospects.Biomolecules. 2020 Oct 27;10(11):1487. doi: 10.3390/biom10111487. Biomolecules. 2020. PMID: 33121065 Free PMC article. Review.
-
Traumatic brain injury (TBI) in collision sports: Possible mechanisms of transformation into chronic traumatic encephalopathy (CTE).Metabolism. 2019 Nov;100S:153943. doi: 10.1016/j.metabol.2019.07.007. Metabolism. 2019. PMID: 31610856 Review.
-
Does neuroinflammation drive the relationship between tau hyperphosphorylation and dementia development following traumatic brain injury?Brain Behav Immun. 2017 Feb;60:369-382. doi: 10.1016/j.bbi.2016.09.027. Epub 2016 Sep 28. Brain Behav Immun. 2017. PMID: 27686843 Review.
-
Association between single moderate to severe traumatic brain injury and long-term tauopathy in humans and preclinical animal models: a systematic narrative review of the literature.Acta Neuropathol Commun. 2022 Jan 31;10(1):13. doi: 10.1186/s40478-022-01311-0. Acta Neuropathol Commun. 2022. PMID: 35101132 Free PMC article.
-
Assembly of recombinant tau into filaments identical to those of Alzheimer's disease and chronic traumatic encephalopathy.Elife. 2022 Mar 4;11:e76494. doi: 10.7554/eLife.76494. Elife. 2022. PMID: 35244536 Free PMC article.
Cited by
-
Zebrafish as an Innovative Tool for Epilepsy Modeling: State of the Art and Potential Future Directions.Int J Mol Sci. 2023 Apr 22;24(9):7702. doi: 10.3390/ijms24097702. Int J Mol Sci. 2023. PMID: 37175408 Free PMC article. Review.
-
Acute Treatment with the M-Channel (Kv7, KCNQ) Opener Retigabine Reduces the Long-Term Effects of Repetitive Blast Traumatic Brain Injuries.Neurotherapeutics. 2023 Apr;20(3):853-869. doi: 10.1007/s13311-023-01361-9. Epub 2023 Mar 28. Neurotherapeutics. 2023. PMID: 36976493
-
Abusive Head Trauma Animal Models: Focus on Biomarkers.Int J Mol Sci. 2023 Feb 24;24(5):4463. doi: 10.3390/ijms24054463. Int J Mol Sci. 2023. PMID: 36901893 Free PMC article. Review.
-
Longitudinal in vivo imaging of adult Danionella cerebrum using standard confocal microscopy.Dis Model Mech. 2022 Dec 1;15(12):dmm049753. doi: 10.1242/dmm.049753. Epub 2022 Dec 22. Dis Model Mech. 2022. PMID: 36398624 Free PMC article.
-
Neurons derived from individual early Alzheimer's disease patients reflect their clinical vulnerability.Brain Commun. 2022 Oct 21;4(6):fcac267. doi: 10.1093/braincomms/fcac267. eCollection 2022. Brain Commun. 2022. PMID: 36349119 Free PMC article.
References
Publication types
MeSH terms
Substances
Grant support
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials

